Lassa fever, also known as Lassa hemorrhagic fever (LHF), is a type of viral hemorrhagic fever caused by the Lassa virus. The natural reservoir for the virus is that the Mastomys natalensis rodent (commonly referred to as the multimammate rat). Lassa mammarenavirus is an emerging virus and a select agent, requiring Biosafety Level 4-equivalent containment.
- Scientific name: Lassa virus
- Rank: Species
- Higher classification: Arenavirus
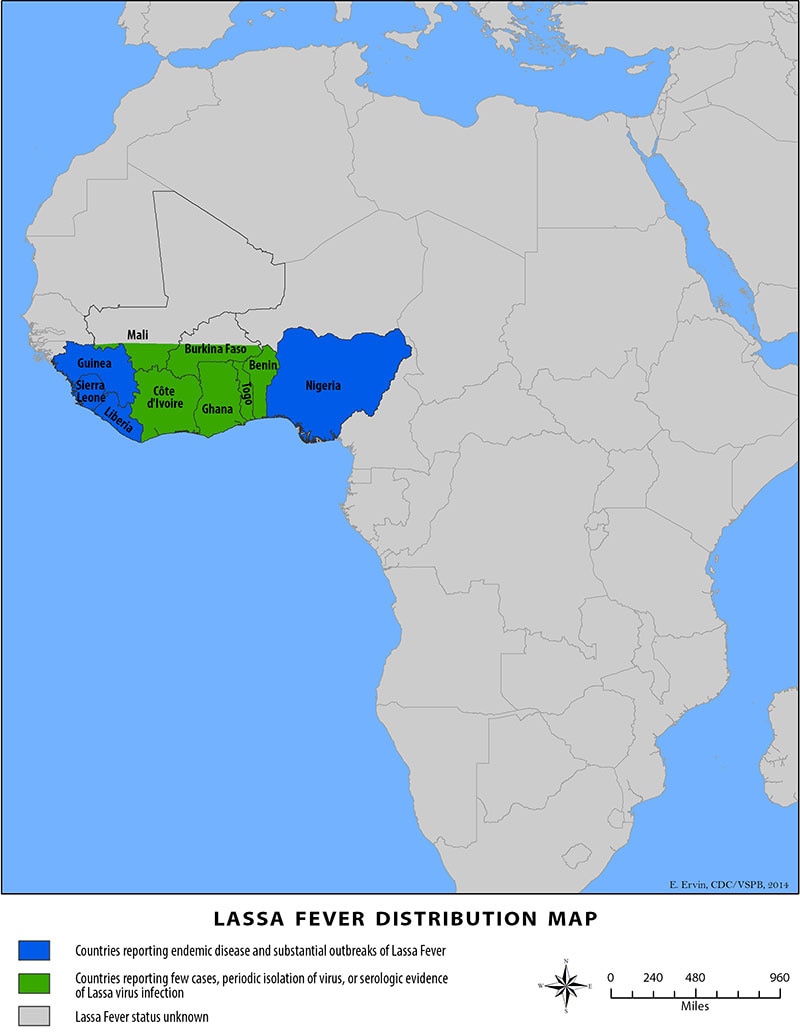
Lassa fever remains a serious public health challenge in West Africa with Nigeria bearing the very best burden. Lassa fever occurs throughout the year but more cases are recorded during the season i.e. November through May.
The disease is usually initially spread to people via:
1. Direct contact with urine, faces, saliva or blood of infected rats.
2. Contact with objects, home items and surfaces or eating food, contaminated with urine, faeces, saliva or blood of infected rats.
3. Person to person transmission by contact with blood, urine, faeces, vomitus, and other body fluids of an infected person.
Signs and symptoms of Lassa fever:
Lassa fever typically occur 1-3 weeks after the patient comes into contact with the virus. For the majority of Lassa fever virus infections (approximately 80%), symptoms are mild and are undiagnosed. Mild symptoms include fever, headache, pharyngitis , general body weakness, cough, nausea, vomiting, diarrhoea, muscle pains, pain , and in severe cases, unexplainable bleeding from ears, eyes, nose, mouth and other body openings.. In 20% of infected individuals, however, disease may progress to more serious symptoms including hemorrhaging (in gums, eyes, or nose, as examples), respiratory distress, repeated vomiting, facial swelling, pain in the chest, back, and abdomen, and shock. Neurological problems have also been described, including hearing loss, tremors, and encephalitis. Death may occur within two weeks after symptom onset due to multi-organ failure.
Early treatment and diagnosis increases the probabilities of survival. People most in danger are:
- People of all age groups who are available contact with the urine, faeces, saliva or blood of rats
- People living in rat infested environments which increases their chances of coming in contact with rats
- people that consume potentially contaminated food stuff especially those left open overnight or dried outside within the open
- people that handle or process rodents for consumption
- people that don’t perform hand hygiene when appropriate
- Relatives who look after diseased person with unexplained illnesses reception
- Health care workers including: Doctors, nurses and other doctors providing direct patient care within the absence of ordinary precautions.
- Hospital staff who clean and disinfect contaminated surfaces, materials and supplies without adequate protective gear
- Laboratory staff who handle blood samples of suspected Lassa fever patients without appropriate precautions
Medical or support staff who prepare and or handle dead bodies without appropriate precautions.
The most common complication of Lassa fever is deafness. Various degrees of deafness occur in approximately one-third of infections, and in many cases hearing loss is permanent. As far as is known, severity of the disease does not affect this complication: deafness may develop in mild as well as in severe cases.
To reduce the danger of Lassa fever , the Nigeria Centre for Disease Control (NCDC) offers the following advice:
• Ensure proper environmental sanitation – i.e. keep your environment clean in the least times, block all holes in your house to stop rats from entry.
• Cover your dustbins and dispose refuse properly. Communities should setup dump sites very faraway from their homes to scale back the probabilities of getting rodents within homes
• Store foodstuff like rice, garri, beans, corn/maize etc. containers which are well covered with tight fitting lids
• Avoid drying food stuff outside on the ground , roadside where it’ll be exposed to contamination
• Avoid bush burning which may cause displacement of rats from bushes to human dwellings
• Eliminate rats in homes and communities by setting rat traps and other means
• Practice good personal hygiene by frequent washing hands with soap under running water/or use of hand sanitisers when appropriate
• Visit the closest clinic if you notice any of the signs and symptoms of Lassa fever as mentioned earlier, avoid self-medication
• Healthcare workers are advised to practice standard precautions in the least times: i.e. wearing gloves while handling patients or providing care to an ill patient/relative.
• Healthcare workers should maintain a high index of suspicion for Lassa fever i.e. be vigilant and lookout for signs and symptoms of Lassa fever .
TREATMENT
Ribavirin, an antiviral drug, has been used with success in Lassa fever patients. It has been shown to be most effective when given early in the course of the illness. Patients should also receive supportive care consisting of maintenance of appropriate fluid and electrolyte balance, oxygenation and blood pressure, as well as treatment of any other complicating infections.
Any febrile illness that has not skilled 48 hours use of anti-malaria or antibiotics should raise an index of suspicion for Lassa fever ! Please if your healthcare worker suspects Lassa fever, advise him or her to contact your government disease surveillance and notification officer to access care in Nigeria.